TMJ Guide
Pelvic Floor Exercises After Birth: Recovery Plan
Expert guide on pelvic-floor-exercises-after-birth
By Dr. Emily Watson, Women's Health Physiotherapist · Published 2026-03-10 · Updated 2026-03-10

By Dr. Emily Watson, Women's Health Physiotherapist | Last updated: March 2026
After giving birth, around 1 in 3 women experience pelvic floor dysfunction. Pelvic floor exercises after birth help restore muscle strength, prevent urinary incontinence, and support long-term core recovery. This guide covers 10 progressive exercises, when to start safely, and signs you may need professional help from a pelvic floor physiotherapist.
Table of Contents
- Why Does the Pelvic Floor Weaken After Birth?
- When Can You Start Pelvic Floor Exercises After Birth?
- 10 Pelvic Floor Exercises After Birth: Complete Progression
- Exercise Progression Table by Week
- Signs You Need a Pelvic Floor Physiotherapist
- Best Products for Pelvic Floor Recovery
- Tips for Staying Consistent
- Frequently Asked Questions
- Sources
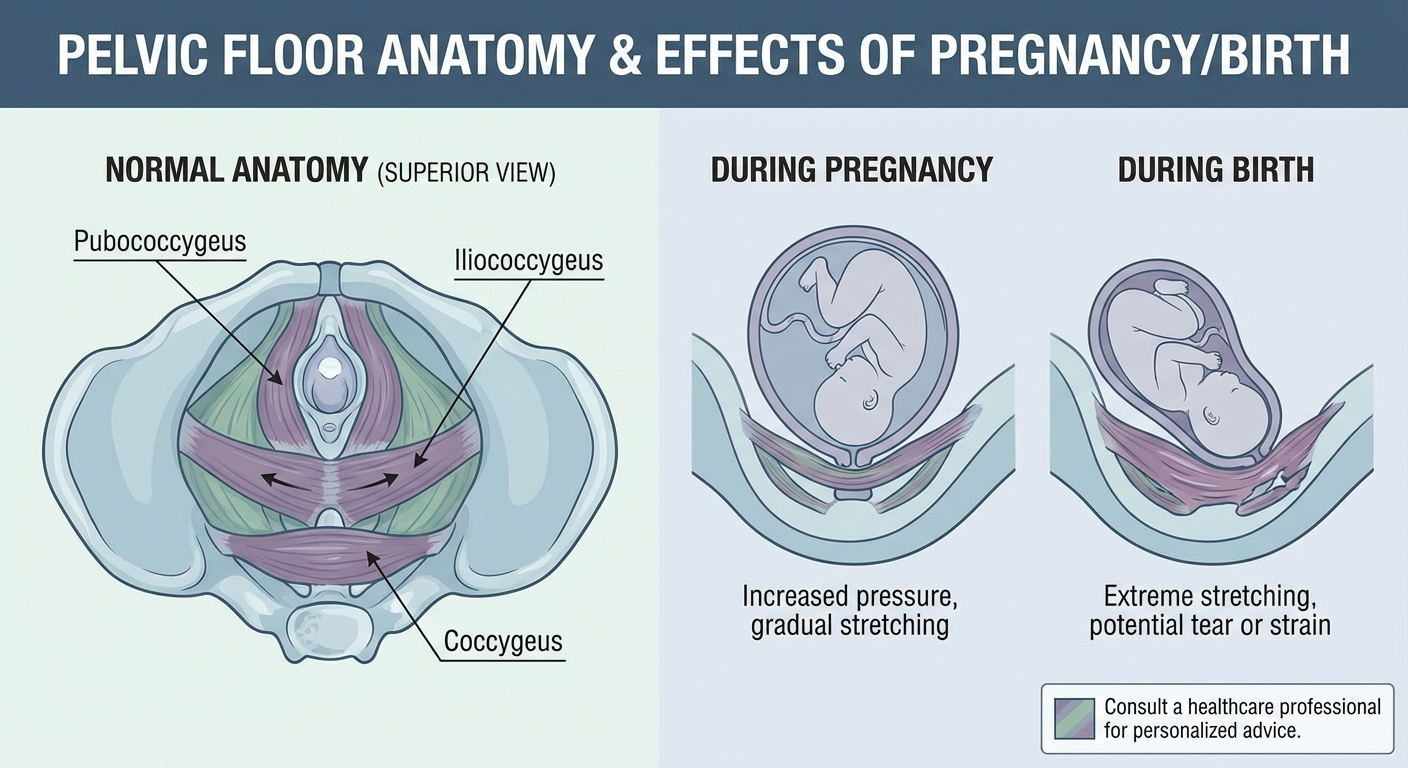
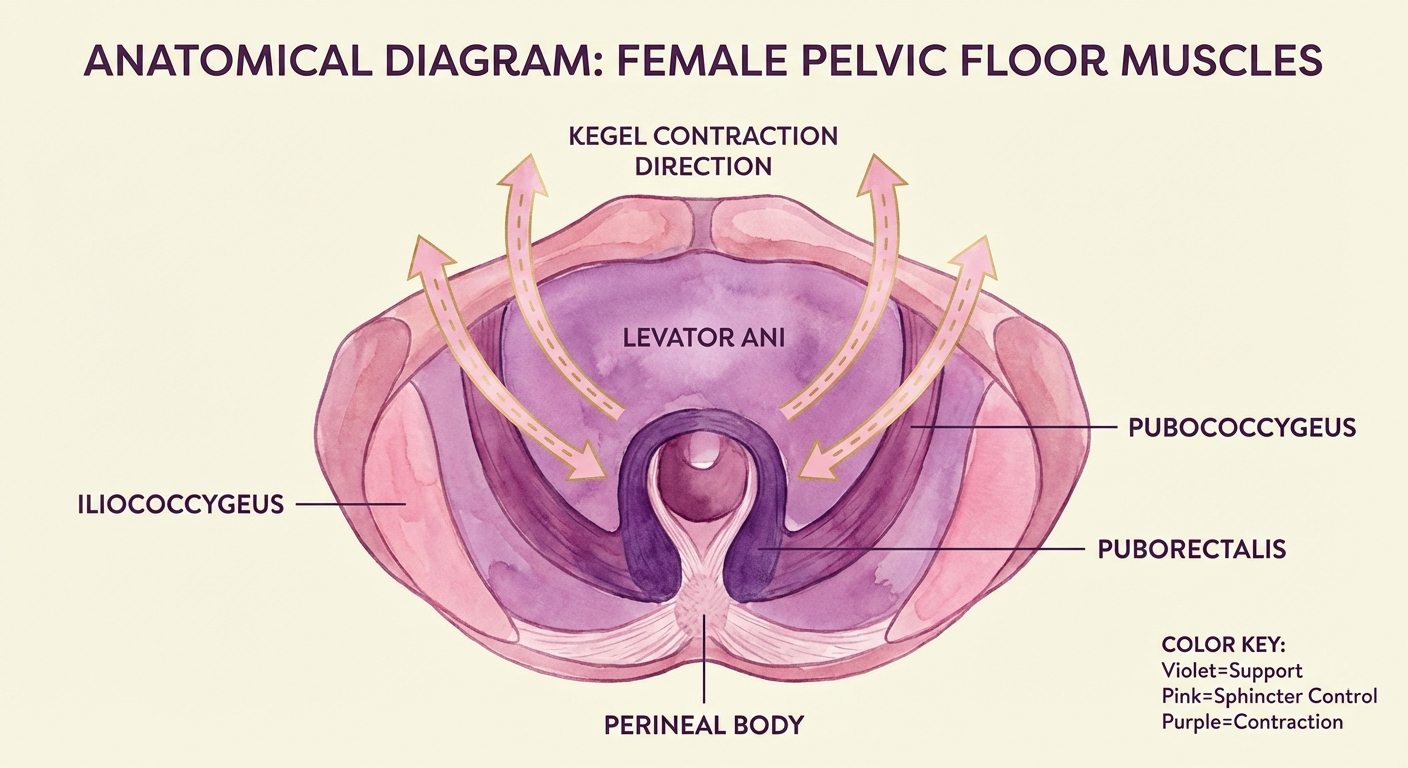
Why Does the Pelvic Floor Weaken After Birth?
The pelvic floor is a hammock-shaped group of muscles that stretches from your pubic bone to your tailbone. These muscles support your bladder, uterus, and bowel. During pregnancy and birth, they undergo extraordinary strain — and understanding why they weaken is the first step toward effective recovery.
The Impact of Pregnancy
Even before delivery, your pelvic floor has been working overtime. Throughout nine months of pregnancy, these muscles support the growing weight of your baby, placenta, and amniotic fluid. The hormone relaxin softens connective tissues and ligaments, making them more flexible for birth but also more vulnerable to weakness. Research published in the International Urogynecology Journal shows that up to 35% of women develop some degree of pelvic floor dysfunction during pregnancy alone.
The Impact of Vaginal Delivery
During vaginal delivery, the pelvic floor muscles stretch up to three times their resting length. This can cause micro-tears, nerve damage, and significant muscle fatigue. Factors that increase pelvic floor trauma include prolonged pushing stages, assisted delivery with forceps or vacuum, delivering a baby over 4kg (8.8 lbs), and perineal tearing or episiotomy.
After Caesarean Section
If you had a caesarean birth, you might assume your pelvic floor is unaffected. However, the weight of pregnancy itself causes significant strain. Studies show that women who deliver by caesarean still have elevated rates of urinary incontinence compared to women who have never been pregnant. As outlined in our postpartum recovery guide, recovery after any type of birth requires intentional rehabilitation.
What Pelvic Floor Weakness Feels Like
Common symptoms of a weakened pelvic floor include:
- Stress urinary incontinence — leaking when you cough, sneeze, laugh, or jump
- Urge incontinence — a sudden, strong need to urinate that is hard to delay
- Heaviness or dragging in the vaginal area (a sign of potential prolapse)
- Reduced sensation during intimacy
- Difficulty controlling wind
- Lower back pain that does not respond to typical treatments
Around 50% of women who have given birth experience at least one of these symptoms in the first year postpartum. The good news is that targeted pelvic floor exercises after birth can significantly improve — and often fully resolve — these issues.
When Can You Start Pelvic Floor Exercises After Birth?

One of the most common questions new mums ask is when it is safe to begin exercising the pelvic floor. The answer may be sooner than you think.
After Vaginal Birth
You can begin gentle pelvic floor exercises within 24 to 48 hours of a vaginal delivery, as long as you are comfortable. In fact, the Royal College of Obstetricians and Gynaecologists (RCOG) recommends starting gentle Kegel contractions as soon as possible after birth. These early contractions help increase blood flow to the perineum, which supports tissue healing.
Start with very gentle contractions — you may not feel much at first, and that is completely normal. Think of it as sending a signal to your muscles to "wake up" rather than expecting a strong squeeze.
After Caesarean Birth
After a caesarean section, you can typically begin gentle pelvic floor exercises once your catheter has been removed and you feel comfortable. This is usually within 24 to 48 hours of surgery. Avoid any exercises that strain your abdominal incision. Our postpartum recovery guide covers the broader timeline for post-caesarean healing in detail.
The Six-Week Check
Your six-week postnatal check-up is an important milestone. At this appointment, discuss your pelvic floor recovery with your GP or midwife. However, do not wait until this appointment to begin gentle exercises — the earlier you start, the better your outcomes tend to be.
After six weeks (and with your healthcare provider's clearance), you can begin progressing to more challenging exercises and eventually return to higher-impact activities.
10 Pelvic Floor Exercises After Birth: Complete Progression
These 10 exercises are arranged from gentlest to most advanced. Begin with Exercises 1 through 3 in the early days, and progress gradually as your strength improves. Quality always matters more than quantity — a correct, well-executed contraction is far more valuable than rushing through repetitions.
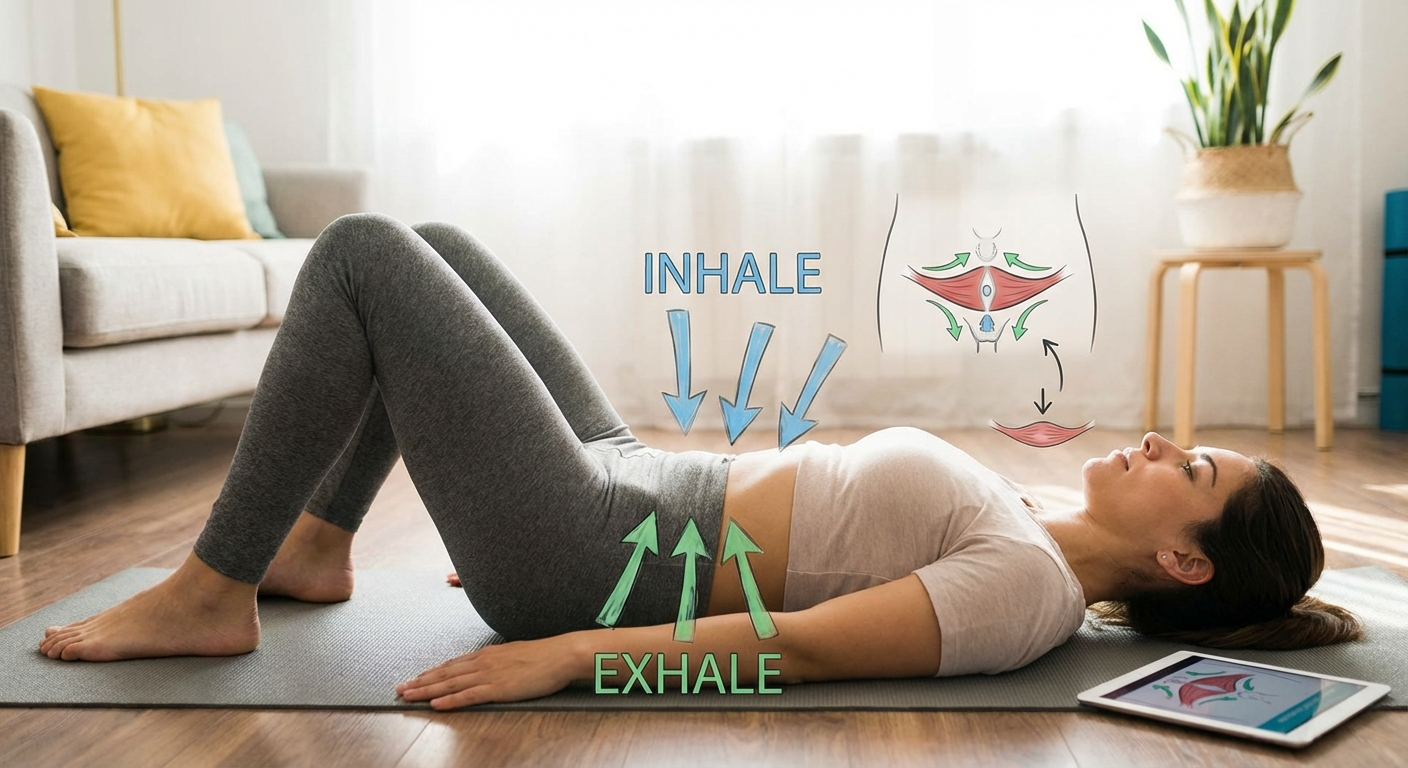
Exercise 1: Gentle Pelvic Floor Activation (Week 1+)
This is your starting point. You can do this lying down, which removes gravity from the equation.
How to do it:
- Lie on your back with knees bent and feet flat on the floor (or bed).
- Take a relaxed breath in.
- As you exhale, gently squeeze your pelvic floor muscles — imagine you are stopping the flow of urine and holding in wind at the same time.
- Hold for 1 to 2 seconds.
- Fully release and rest for 5 seconds.
- Repeat 5 times, 3 times per day.
Key tip: If you cannot feel any contraction at all, do not worry. Simply visualising the squeeze sends neural signals that begin the recovery process.
Exercise 2: Quick Flick Contractions (Week 1+)
These target your fast-twitch muscle fibres, which are responsible for stopping sudden leaks when you cough or sneeze.
How to do it:
- Lie comfortably on your back.
- Quickly squeeze and release your pelvic floor muscles — think of a quick "pulse."
- Each squeeze-and-release should take about 1 second.
- Perform 10 quick flicks, rest for 10 seconds.
- Repeat 3 sets, twice per day.
Key tip: Keep your buttocks, thighs, and abdominals relaxed. The movement should come entirely from the pelvic floor.
Exercise 3: Sustained Hold with Breathing (Week 2+)
Once you can feel a gentle contraction, begin building endurance with longer holds.
How to do it:
- Lie on your back with knees bent.
- Inhale to prepare.
- As you exhale, contract your pelvic floor and hold for 3 to 5 seconds.
- Breathe normally while holding.
- Release fully and rest for 10 seconds.
- Repeat 8 times, 3 times per day.
Key tip: If you lose the contraction before the full hold time, simply hold for as long as you can and build up gradually.
Exercise 4: Seated Pelvic Floor Contractions (Week 3+)
Moving to a seated position adds gravity, which makes the exercise more challenging.
How to do it:
- Sit upright on a firm chair with feet flat on the floor.
- Exhale and contract your pelvic floor, lifting and squeezing inward.
- Hold for 5 seconds.
- Release fully and rest for 5 seconds.
- Repeat 10 times, twice per day.
Key tip: Sitting on a rolled-up towel can help you feel the contraction more clearly.
Exercise 5: Standing Pelvic Floor Holds (Week 4+)
Standing is the most functional position — this is how your pelvic floor works in daily life.
How to do it:
- Stand with feet hip-width apart, weight evenly distributed.
- Exhale and contract your pelvic floor muscles.
- Hold for 5 to 8 seconds.
- Release and rest for 5 seconds.
- Repeat 10 times, twice per day.
Key tip: Try doing these while waiting for the kettle to boil or standing at the kitchen counter. Building them into daily routines helps with consistency.
Exercise 6: Heel Slides with Pelvic Floor Engagement (Week 4+)
This exercise combines pelvic floor activation with gentle core movement, building coordination between the two muscle groups.
How to do it:
- Lie on your back with knees bent and feet flat.
- Exhale, contract your pelvic floor, and slowly slide one heel along the floor until the leg is straight.
- Inhale and slide the heel back to the starting position while maintaining the pelvic floor contraction.
- Release the pelvic floor.
- Repeat 8 times on each side, twice per day.
Key tip: If you feel any downward pressure or bulging in your pelvic floor, reduce the range of motion or go back to the previous exercise for another week.
Exercise 7: Bridge with Pelvic Floor Activation (Week 5+)
The bridge strengthens your glutes and pelvic floor simultaneously — two muscle groups that work closely together. Many women find that wearing a supportive best postpartum belly wrap during these exercises provides additional comfort and confidence.
How to do it:
- Lie on your back with knees bent and feet flat, hip-width apart.
- Exhale, contract your pelvic floor, and slowly lift your hips off the floor until your body forms a straight line from knees to shoulders.
- Hold at the top for 3 to 5 seconds, keeping the pelvic floor engaged.
- Slowly lower back down.
- Release the pelvic floor.
- Repeat 10 times, twice per day.
Key tip: Avoid arching your lower back at the top of the bridge. Think about tucking your tailbone slightly.
Exercise 8: The Elevator (Week 6+)
This advanced contraction exercise builds layered control and awareness of different levels of pelvic floor tension.
How to do it:
- Sit or lie comfortably.
- Imagine your pelvic floor is a lift (elevator) in a building.
- Exhale and contract to the "first floor" — a gentle, 25% squeeze. Hold for 2 seconds.
- Contract further to the "second floor" — a 50% squeeze. Hold for 2 seconds.
- Contract to the "third floor" — a 75% squeeze. Hold for 2 seconds.
- Contract to the "top floor" — your maximum squeeze. Hold for 2 seconds.
- Slowly release back down floor by floor.
- Repeat 5 times, once per day.
Key tip: This exercise takes real concentration. Start with just 2 to 3 "floors" and build up as your awareness improves.
Exercise 9: Squat with Pelvic Floor Focus (Week 8+)
Squats are one of the most functional movements you will perform as a new mum — picking up your baby, lifting car seats, and getting up from the floor all involve squatting.
How to do it:
- Stand with feet slightly wider than hip-width apart.
- Inhale as you lower into a squat, allowing the pelvic floor to lengthen and relax.
- Exhale as you stand back up, contracting the pelvic floor as you rise.
- Repeat 10 times, twice per day.
Key tip: Only squat as low as feels comfortable. You do not need to go below parallel, especially in the early months.
Exercise 10: Single-Leg Balance with Pelvic Floor Hold (Week 10+)
This advanced exercise challenges your pelvic floor in an unstable position, preparing you for return to running and higher-impact activities.
How to do it:
- Stand near a wall or chair for balance support.
- Contract your pelvic floor.
- Slowly lift one foot off the floor, maintaining your pelvic floor contraction.
- Hold for 10 to 15 seconds.
- Lower your foot and release the pelvic floor.
- Repeat 5 times on each side, once per day.
Key tip: If you wobble, that is fine — the wobble is actually making your deep stabilisers work harder. Use the wall if you need to.
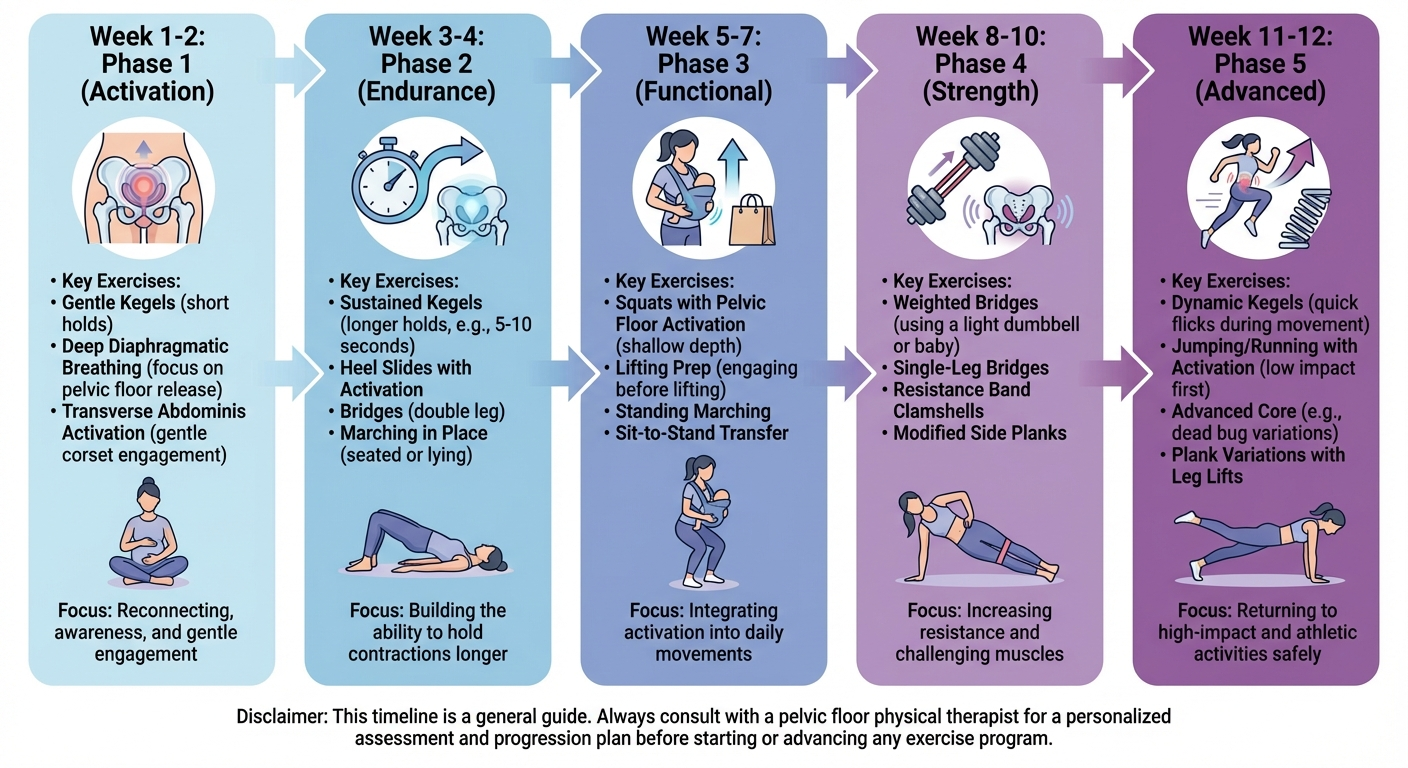
Exercise Progression Table by Week
This table provides a clear roadmap for your pelvic floor recovery. Always listen to your body and progress only when the current phase feels comfortable and controlled.
| Phase | Weeks Postpartum | Exercises | Sets x Reps | Position | Notes |
|---|---|---|---|---|---|
| Phase 1: Activation | Week 1–2 | 1. Gentle Activation, 2. Quick Flicks | 3 x 5–10 | Lying down | Focus on finding the contraction; no pressure for perfection |
| Phase 2: Endurance | Week 2–4 | 3. Sustained Hold, 4. Seated Contractions | 3 x 8–10 | Lying/Seated | Build hold time from 3 to 5 seconds gradually |
| Phase 3: Functional | Week 4–6 | 5. Standing Holds, 6. Heel Slides | 2 x 8–10 | Standing/Lying | Add gravity challenge; coordinate with breathing |
| Phase 4: Strength | Week 6–8 | 7. Bridge, 8. Elevator | 2 x 5–10 | Lying/Seated | Combine pelvic floor with glute and core work |
| Phase 5: Advanced | Week 8–12+ | 9. Squat, 10. Single-Leg Balance | 2 x 5–10 | Standing | Prepare for return to exercise and higher-impact activity |
Important: If you had a third- or fourth-degree tear, an assisted delivery, or a caesarean section, your progression may be slower. This is completely normal. Always follow the guidance of your healthcare provider and consider working with a pelvic floor physiotherapist for a personalised plan. Our postpartum recovery guide has more detailed timelines based on your type of delivery.
Signs You Need a Pelvic Floor Physiotherapist
While many women recover well with a home exercise programme, there are situations where professional support is essential. A women's health physiotherapist can perform an internal assessment, identify specific muscle weaknesses, and create a tailored rehabilitation plan.
See a pelvic floor physiotherapist if you experience:
- Urinary or faecal incontinence that persists beyond 3 months postpartum
- A feeling of heaviness, pressure, or "something falling out" of the vagina (possible prolapse)
- Pain during intimacy that does not improve over time
- Inability to feel any pelvic floor contraction after several weeks of trying
- Recurrent urinary tract infections
- Ongoing lower back or pelvic pain
- Separation of the abdominal muscles (diastasis recti) greater than 2 finger-widths
According to a 2023 study in The Lancet, structured pelvic floor muscle training with physiotherapist supervision results in a 56% greater reduction in incontinence symptoms compared to unsupervised exercise alone. If you are unsure whether your symptoms warrant professional help, it is always better to seek an assessment — early intervention leads to better outcomes.
A good pelvic floor physiotherapist will also assess how your pelvic floor works in coordination with your deep abdominals, diaphragm, and back muscles. Recovery is never just about one muscle group. You may also benefit from complementary support such as a best postpartum belly wrap, which can provide gentle compression and support to your abdominal wall as you rebuild strength.
Best Products for Pelvic Floor Recovery

While exercises alone are highly effective, several products can support and enhance your pelvic floor recovery journey.
Kegel Trainers
Kegel trainers provide biofeedback, which helps you confirm you are contracting the correct muscles. Many women find they accelerate progress because the device provides real-time feedback on squeeze strength and duration. Look for trainers that connect to a smartphone app for guided programmes and progress tracking.
Popular options include the Elvie Trainer, Perifit, and weighted Kegel exercise sets. Clinical research supports the use of biofeedback devices, with studies showing up to 70% improvement in pelvic floor strength when used alongside a regular exercise programme.
Exercise Balls (Swiss Balls)
A Swiss ball is a versatile tool for postpartum recovery. Sitting on an exercise ball naturally engages your pelvic floor and deep core muscles. You can also use it for gentle bouncing, which encourages pelvic floor activation, and for supported bridge exercises.
Shop Postpartum Exercise Balls on Amazon
When to Introduce Products
Most physiotherapists recommend waiting until at least 6 weeks postpartum before introducing internal Kegel trainers. External tools like exercise balls and resistance bands can be used earlier, as long as you have clearance from your healthcare provider. A supportive best postpartum belly wrap can be worn from the early days to provide gentle abdominal support during your recovery.
Tips for Staying Consistent
Consistency is the single most important factor in pelvic floor recovery. Research shows that women who perform pelvic floor exercises at least 3 times per day see significantly better outcomes than those who exercise sporadically.
Here are practical strategies for building a lasting habit:
- Anchor to existing routines. Do your exercises every time you feed your baby — whether breastfeeding or bottle-feeding, you are sitting still anyway.
- Set phone reminders. Three gentle reminders spread throughout the day can make a real difference.
- Use an app. Apps like Squeezy (developed by NHS physiotherapists) or the Elvie app provide guided programmes and reminders.
- Track your progress. Even a simple tick on a calendar builds momentum and motivation.
- Be patient with yourself. Recovery takes time. Most women notice meaningful improvement by 3 months and significant strength gains by 6 months.
- Involve your partner. Let them know what you are working on so they can support you and give you the time and space for your exercises.
Remember that pelvic floor recovery is a marathon, not a sprint. Some days you will forget. Some days you will not feel like doing them. That is perfectly normal. What matters is getting back to your routine the next day. For a holistic approach to your recovery, our postpartum recovery guide covers nutrition, sleep, and emotional wellbeing alongside physical rehabilitation.
Frequently Asked Questions
How long does it take for pelvic floor exercises to work after birth?
Most women begin to notice improvement in pelvic floor strength within 3 to 6 weeks of consistent daily exercise. However, full recovery typically takes 3 to 6 months. According to the Continence Foundation of Australia, 80% of women who perform regular pelvic floor exercises see significant improvement in incontinence symptoms within 5 months. The key is consistency — performing exercises at least 3 times per day for the best results.
Can I do pelvic floor exercises after a C-section?
Yes, you can and should do pelvic floor exercises after a caesarean section. Even though your pelvic floor was not stretched during vaginal delivery, the weight of pregnancy itself weakens these muscles. You can begin gentle pelvic floor contractions (Exercises 1 and 2 in this guide) once your catheter has been removed, usually within 24 to 48 hours of surgery. Avoid exercises that strain your abdominal incision, and progress more gradually through the phases.
How do I know if I am doing pelvic floor exercises correctly?
You should feel a gentle squeeze and lift inside the vagina and around the back passage. You should not be holding your breath, clenching your buttocks, squeezing your thighs together, or bearing down. One way to check is to insert a clean finger into the vagina and squeeze — you should feel a gentle tightening around your finger. If you are unsure, a women's health physiotherapist can perform an assessment and confirm you are using the correct technique.
Is it normal to leak urine after having a baby?
Urinary leakage is extremely common after birth, affecting up to 1 in 3 new mothers. While it is common, it is not something you simply have to live with. Stress urinary incontinence (leaking when you cough, sneeze, laugh, or exercise) usually improves significantly with regular pelvic floor exercises. If leaking persists beyond 3 months postpartum despite consistent exercise, consult a pelvic floor physiotherapist for specialist assessment and treatment.
When can I return to running or high-impact exercise after birth?
Current guidelines from leading physiotherapy bodies recommend waiting until at least 12 weeks postpartum before returning to running or high-impact exercise. Before you return, you should be able to complete 10 pelvic floor contractions held for 10 seconds each, 10 quick-flick contractions, walk briskly for 30 minutes without pelvic symptoms, and perform single-leg balance for 20 seconds. If you experience any leaking, heaviness, or pain during or after running, these are signs your pelvic floor is not yet ready for that level of impact.
Do pelvic floor exercises help with prolapse after birth?
Pelvic floor exercises are the first-line treatment for mild to moderate pelvic organ prolapse. Research published in The BMJ shows that structured pelvic floor muscle training can reduce prolapse symptoms by one grade in many women. However, prolapse requires professional assessment — if you feel a bulge or heaviness in your vagina, see a women's health physiotherapist or your GP before starting exercises, as you may need a tailored programme.
Sources
-
Woodley, S.J., et al. (2020). "Pelvic floor muscle training for prevention and treatment of urinary and faecal incontinence in antenatal and postnatal women." Cochrane Database of Systematic Reviews. DOI: 10.1002/14651858.CD007471.pub4
-
Royal College of Obstetricians and Gynaecologists (RCOG). (2020). "Pelvic floor exercises after childbirth." Patient Information Leaflet. rcog.org.uk
-
Dumoulin, C., et al. (2018). "Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women." Cochrane Database of Systematic Reviews. DOI: 10.1002/14651858.CD005654.pub4
-
Mørkved, S., & Bø, K. (2014). "Effect of pelvic floor muscle training during pregnancy and after childbirth on prevention and treatment of urinary incontinence: a systematic review." British Journal of Sports Medicine, 48(4), 299–310.
-
Hagen, S., et al. (2014). "Individualised pelvic floor muscle training in women with pelvic organ prolapse (POPPY): a multicentre randomised controlled trial." The Lancet, 383(9919), 796–806.
-
Continence Foundation of Australia. (2023). "Pelvic Floor Muscles — What You Need to Know." continence.org.au
-
Goom, T., Donnelly, G., & Brockwell, E. (2019). "Returning to Running Postnatal — Guidelines for Medical, Health, and Fitness Professionals Managing this Population." Published guidance for postnatal return to running.
-
National Institute for Health and Care Excellence (NICE). (2019). "Urinary incontinence and pelvic organ prolapse in women: management." NICE guideline NG123. nice.org.uk
Visual Guide Gallery
Walking Pad vs Treadmill
30-second comparison