TMJ Guide
Postpartum Recovery: Week-by-Week Guide for New Mums
Expert guide on postpartum-recovery-guide
By Dr. Emily Watson, Women's Health Physiotherapist · Published 2026-03-10 · Updated 2026-03-10

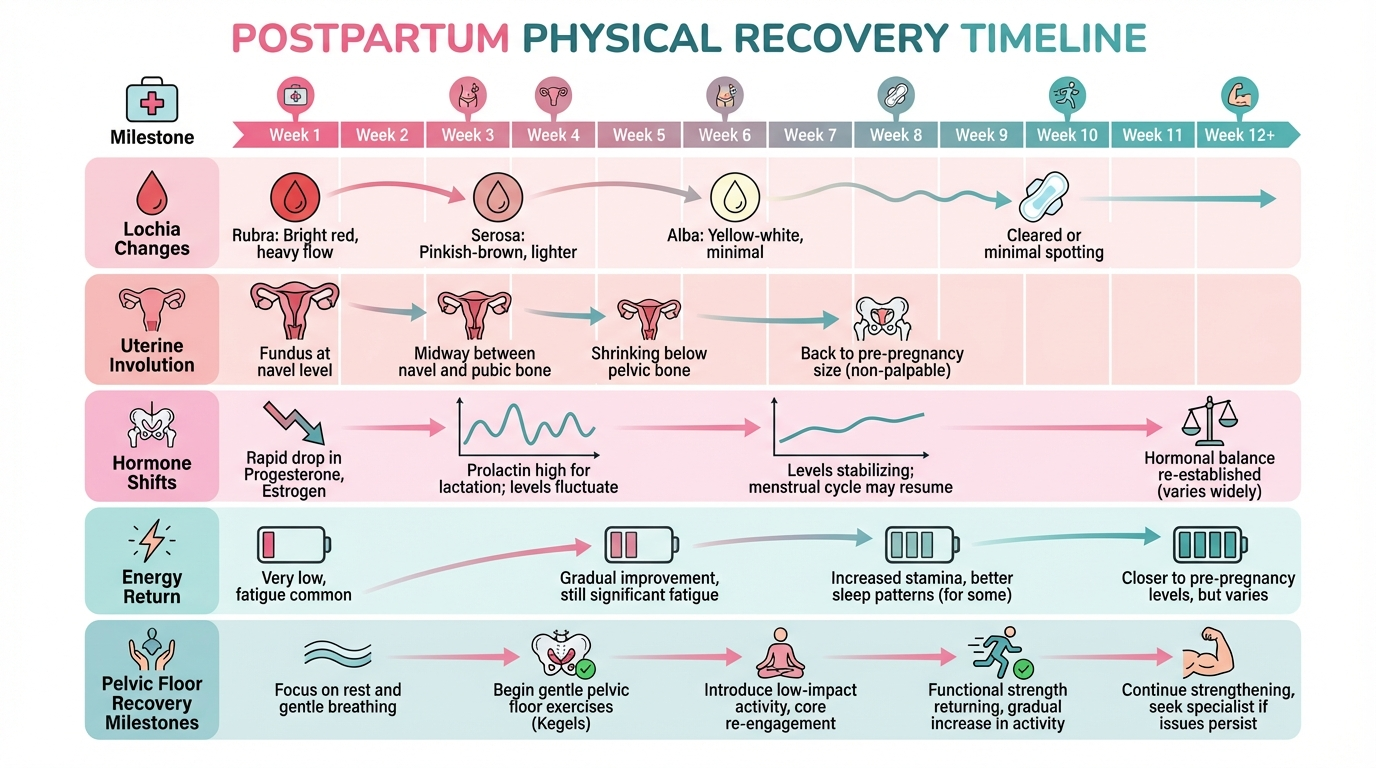
Your body just did something extraordinary. Postpartum recovery typically spans 6 to 12 weeks, though full healing can take up to a year. This week-by-week guide covers what to expect physically and emotionally, when to seek help, and how to support your body at every stage — so you can recover with confidence.
By Dr. Emily Watson, Women's Health Physiotherapist | Last updated: March 2026
Table of Contents

- What Is Postpartum Recovery?
- Week 1: The First Days After Birth
- Week 2: Early Healing Continues
- Weeks 3–4: Finding a New Rhythm
- Weeks 5–6: The Midpoint Milestone
- Weeks 7–8: Rebuilding Strength
- Weeks 9–12: Turning a Corner
- Postpartum Warning Signs You Should Never Ignore
- Postpartum Exercise Progression
- Pelvic Floor Recovery After Birth
- Postpartum Mental Health
- Postpartum Recovery Essentials
- FAQ: Postpartum Recovery
- Sources
What Is Postpartum Recovery?
Postpartum recovery refers to the period after childbirth when your body heals, adjusts, and begins returning to its pre-pregnancy state. According to the American College of Obstetricians and Gynecologists (ACOG), the postpartum period — sometimes called the "fourth trimester" — lasts at least 12 weeks, though many physical and emotional changes continue for months beyond that.
During this time, your uterus shrinks back to its original size, hormone levels shift dramatically, and tissues that stretched or tore during delivery begin to repair. Around 85% of women experience some form of perineal trauma during vaginal birth, and roughly 1 in 3 births in the UK and US are by caesarean section — each pathway comes with its own recovery timeline.
The most important thing to understand is this: postpartum recovery is not a race. Every woman heals at a different pace, and comparing your journey to someone else's is neither fair nor helpful. This guide from PostpartumPath.com is here to give you a realistic, week-by-week framework so you know what is normal, what needs attention, and how to be genuinely kind to yourself along the way.
Week 1: The First Days After Birth

The first week postpartum is the most physically intense stage of recovery. Your body has just completed the enormous task of delivering a baby, and now it shifts immediately into healing mode.
What to Expect Physically
Lochia (postpartum bleeding): You will experience vaginal bleeding regardless of whether you had a vaginal or caesarean birth. In the first few days, this bleeding is typically heavy and bright red, similar to a heavy period. You may pass small clots. This is your uterus shedding its lining and is completely normal.
Uterine cramping (afterpains): Your uterus begins contracting to return to its pre-pregnancy size — a process called involution. These cramps can be surprisingly strong, especially during breastfeeding, as the hormone oxytocin triggers both milk letdown and uterine contractions. Afterpains tend to be more noticeable with second and subsequent babies.
Perineal soreness: If you had a vaginal delivery, the perineal area will be swollen, tender, and possibly stitched. Sitting on a soft cushion, using ice packs wrapped in cloth, and rinsing with warm water after using the toilet can bring real relief. A best postpartum belly wrap can also provide gentle abdominal support during these early days.
Caesarean incision care: If you had a C-section, your incision will be covered with a dressing. You may feel numbness, pulling, or sharp twinges around the area. Avoid lifting anything heavier than your baby, and hold a pillow against your tummy when coughing or laughing.
Breast engorgement: Whether you choose to breastfeed or not, your milk will come in around days 2–5. Your breasts may feel hard, hot, and uncomfortably full. Frequent feeding or expressing, warm compresses before feeds, and cool compresses after can help manage engorgement.
What to Do This Week
- Rest as much as you possibly can. Sleep when baby sleeps is cliché but genuinely wise.
- Accept every offer of help with meals, housework, and older children.
- Stay hydrated — aim for at least 2 litres of water per day.
- Take prescribed pain relief regularly rather than waiting until pain becomes severe.
- Begin gentle pelvic floor activation if comfortable — even a few seconds of "lift and hold" counts. Our full guide to pelvic floor exercises after birth can help you get started safely.
Week 2: Early Healing Continues
By the end of week two, you may notice some small improvements, but healing is still very much underway. Be patient with yourself.
What to Expect Physically
Lochia changes colour: Your postpartum bleeding will likely transition from bright red to a darker brown or pinkish hue. The flow should be gradually decreasing. If it suddenly becomes heavy or bright red again, it may be a sign you are overdoing it — your body is telling you to slow down.
Perineal healing: Stitches, if you had them, are usually dissolving by now. The area may still feel tight, swollen, or itchy as tissue repairs. Warm sitz baths (sitting in a shallow basin of warm water for 10–15 minutes) can be wonderfully soothing.
Night sweats: Hormonal shifts cause many new mums to wake drenched in sweat. This is your body's way of shedding the extra fluid it retained during pregnancy. Keep a spare set of pyjamas and a towel by your bed.
Constipation and haemorrhoids: These remain common in week two. Eat fibre-rich foods, stay hydrated, and use a small stool under your feet on the toilet to reduce straining.
What to Do This Week
- Continue resting, but short, gentle walks around the house or garden are beneficial if you feel up to it.
- Monitor your mood. The "baby blues" — feeling weepy, anxious, or overwhelmed — affect up to 80% of new mothers and typically peak around days 3–5, resolving by week two. If feelings intensify rather than lift, speak to your midwife or GP.
- Keep your caesarean incision clean and dry. Watch for redness, swelling, or discharge that could indicate infection.
Weeks 3–4: Finding a New Rhythm

By weeks three and four, many women start to feel the fog lifting slightly. You are still recovering, but small pockets of energy may return.
What to Expect Physically
Lochia continues to lighten: Bleeding often becomes a yellowish-white discharge called lochia alba. Some women find it stops and starts during this period, which is normal.
Abdominal changes: Your belly will still look and feel different. The uterus is still shrinking and won't return to its pre-pregnancy position until around week six. Diastasis recti — the separation of the abdominal muscles — is present in nearly 100% of women at the end of pregnancy and still significant in about 60% of women at six weeks postpartum. Wearing a supportive best postpartum belly wrap can provide comfort and gentle compression during this period.
Hair texture and skin: You may notice your skin clearing up or breaking out as hormones shift. Postpartum hair loss typically doesn't begin until around month three, so enjoy your thick pregnancy hair a little longer.
What to Do This Week
- Gradually increase short walks if you feel ready. A 10–15 minute walk outdoors can do wonders for both physical recovery and mood.
- Continue pelvic floor exercises daily, gently increasing the duration of holds. Check out our detailed pelvic floor exercises after birth guide for a progressive programme.
- Start thinking about your six-week GP check-up and note any questions or concerns you want to raise.
Weeks 5–6: The Midpoint Milestone
Week six is often treated as a major milestone in postpartum recovery — it is typically when your GP or obstetrician conducts a postnatal check-up. However, it is important to understand that being "cleared" at six weeks does not mean your recovery is complete.
What to Expect Physically
Lochia usually stops: Most women find that postpartum bleeding has ceased entirely by week six, though some light spotting can continue.
Your six-week check-up: This appointment usually includes a check on your caesarean scar or perineal healing, blood pressure, mood screening, and a discussion about contraception. Research published in the BMJ suggests that many women feel this appointment is rushed and does not adequately address their concerns — so prepare your questions in advance and advocate for yourself.
First postpartum period: If you are not breastfeeding exclusively, your period may return as early as six weeks postpartum. If you are breastfeeding, it may be delayed for months. That first period can be heavier or more painful than you remember, which is normal.
What to Do This Week
- Attend your postnatal check-up and be honest about how you are feeling, both physically and emotionally.
- If you have been given the go-ahead, you can begin gentle postnatal exercise (see the exercise progression section below).
- Discuss any persistent pelvic floor symptoms — leaking urine, heaviness, or pain during intimacy — with your GP. These are common but treatable, not something you should simply accept.
Weeks 7–8: Rebuilding Strength

With your six-week check behind you, weeks seven and eight are when many women feel ready to start gently rebuilding their physical strength. The key word is gently.
What to Expect Physically
Energy fluctuations: You may have a good day followed by two exhausting ones. This is normal. Sleep deprivation from night feeds compounds recovery fatigue. According to a 2019 study in Sleep Medicine Reviews, new parents lose an average of 2–3 hours of sleep per night in the first three months.
Caesarean scar tissue: If you had a C-section, your scar may feel tight, numb, or sensitive. Gentle scar massage (once the wound is fully closed and your GP has approved it) can help improve mobility and reduce adhesions.
Core and pelvic floor: Your deep core muscles — including the transverse abdominis and pelvic floor — are the foundation for all other movement. Rebuilding these first is essential before progressing to more demanding exercises.
What to Do This Week
- Focus on postnatal-specific exercises: pelvic tilts, gentle bridges, wall push-ups, and breathing exercises that reconnect your core.
- Walk for 20–30 minutes daily if comfortable.
- Eat nourishing, protein-rich meals to support tissue repair.
Weeks 9–12: Turning a Corner
By weeks nine to twelve, many women notice a genuine shift. Your body feels more like your own again, even if it is different from before.
What to Expect Physically
Diastasis recti improvement: With consistent, appropriate exercise, many women see their abdominal separation begin to narrow. Research from the Norwegian School of Sport Sciences found that targeted exercise programmes can reduce diastasis recti gap width by an average of 35% within 12 weeks.
Hormonal stabilisation: While hormones continue to fluctuate (especially if breastfeeding), the most dramatic shifts have usually settled by now. Your mood may feel more predictable.
Returning to fitness: Around the 12-week mark, most women can begin gradually returning to moderate-intensity exercise — with appropriate guidance and provided they have no ongoing pelvic floor or abdominal issues.
What to Do This Week
- If you experience any pelvic floor symptoms (leaking, heaviness, pain), request a referral to a women's health physiotherapist before increasing exercise intensity.
- Consider a postnatal exercise class designed specifically for recovering mothers.
- Celebrate how far you have come. Twelve weeks of recovery is significant, and you deserve to acknowledge that.
Postpartum Warning Signs You Should Never Ignore
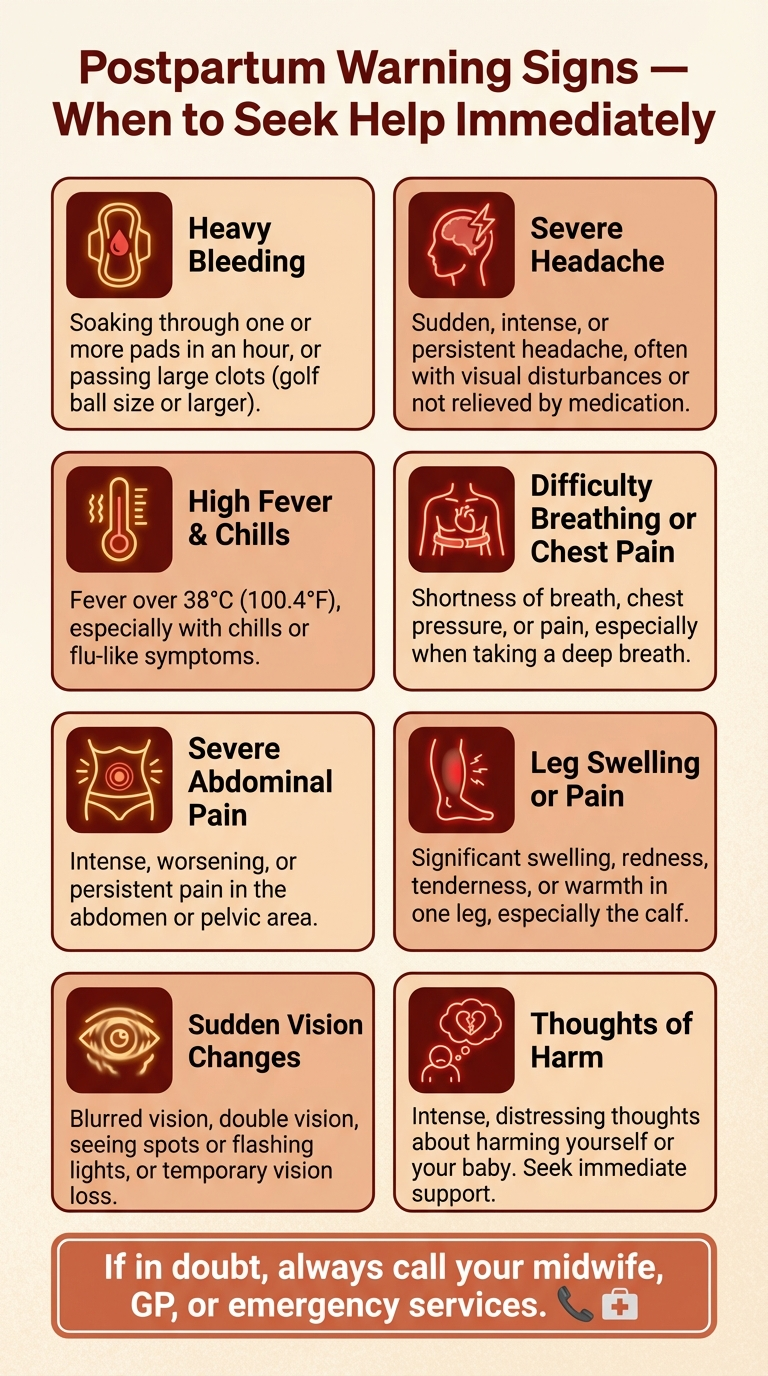
While most postpartum symptoms are normal parts of recovery, some require immediate medical attention. Contact your midwife, GP, or go to A&E / the emergency room if you experience any of the following:
- Heavy bleeding that soaks through a pad in an hour or less, or passing clots larger than a golf ball
- Fever above 38°C (100.4°F) that persists
- Severe headache that does not respond to pain relief, visual disturbances, or upper abdominal pain (these can be signs of postpartum preeclampsia)
- Foul-smelling vaginal discharge which may indicate infection
- Redness, swelling, or discharge from a caesarean incision or perineal stitches
- Painful, red, or hot area on your breast with flu-like symptoms (possible mastitis)
- Calf pain, swelling, or redness in one leg (possible deep vein thrombosis)
- Difficulty breathing or chest pain
- Thoughts of harming yourself or your baby — this is a medical emergency; call 999, 911, or your local emergency number immediately
Postpartum complications are treatable, but early intervention is critical. Trust your instincts — if something feels wrong, it is always worth checking.
Postpartum Exercise Progression
One of the most common questions on PostpartumPath.com is "when can I exercise after having a baby?" The answer depends on several factors, including your type of delivery, any complications, and how your pelvic floor is functioning.
General Timeline for Exercise After Birth
Weeks 1–2: Pelvic floor activation (gentle squeezes), deep breathing, and short walks only.
Weeks 2–6: Gentle walking (increasing distance gradually), pelvic tilts, heel slides, and continued pelvic floor exercises. No impact, no heavy lifting, no abdominal crunches.
Weeks 6–12 (after GP clearance): Postnatal Pilates or yoga, bodyweight exercises (bridges, squats, wall push-ups), swimming (once bleeding has fully stopped and any wounds are healed), and longer walks.
12 weeks and beyond: Gradual return to running, gym work, or group fitness — ideally after a pelvic floor assessment by a women's health physiotherapist. The guidelines published by Gráinne Donnelly and Tom Goom in 2019 recommend waiting until at least 12 weeks postpartum before returning to running, and only after passing specific pelvic floor readiness criteria.
Exercises to Avoid in Early Postpartum Recovery
- Sit-ups, crunches, and traditional planks (these can worsen diastasis recti)
- High-impact activities such as running, jumping, or HIIT
- Heavy weightlifting
- Any exercise that causes pain, leaking, or a feeling of heaviness in the pelvis
The golden rule: if an exercise causes symptoms, stop and step back to a less demanding option. Recovery is not linear, and that is perfectly okay.
Pelvic Floor Recovery After Birth
Your pelvic floor muscles have been under enormous strain during pregnancy and birth. These muscles support your bladder, uterus, and bowel, and they play a vital role in continence, sexual function, and core stability.
Research published in the International Urogynecology Journal found that approximately 1 in 3 women experience some degree of urinary incontinence in the first year after giving birth. The good news is that pelvic floor exercises — when done correctly and consistently — are highly effective at treating and preventing these symptoms.
How to Start Pelvic Floor Exercises
- Find the right muscles: Imagine you are trying to stop the flow of urine and hold in wind at the same time. The muscles you feel lifting and squeezing are your pelvic floor.
- Start gently: Hold for 1–2 seconds, then release fully. Repeat 5 times.
- Build gradually: Work up to holding for 10 seconds, with 10 repetitions, three times per day.
- Add quick flicks: After your holds, do 10 fast squeeze-and-release contractions. These train the muscles that react quickly when you cough or sneeze.
For a complete, progressive programme, visit our dedicated guide: pelvic floor exercises after birth. This is one of the most important things you can do for your long-term health and wellbeing.
If you are unsure whether you are activating the right muscles, or if you have symptoms of prolapse or incontinence, a women's health physiotherapist can assess your pelvic floor and create a tailored rehabilitation plan.
Postpartum Mental Health
Physical recovery gets much of the attention, but postpartum mental health is equally important — and the two are deeply intertwined.
Baby Blues vs. Postnatal Depression
Baby blues affect up to 80% of new mothers and typically appear within the first few days after birth. Symptoms include tearfulness, irritability, anxiety, and mood swings. They usually resolve within two weeks without treatment.
Postnatal depression (PND) is a clinical condition that affects approximately 1 in 7 new mothers, according to data from the CDC and the UK's National Health Service. Symptoms include persistent low mood, loss of interest or pleasure, difficulty bonding with your baby, changes in appetite or sleep (beyond what is caused by the baby), feelings of worthlessness or guilt, and in severe cases, thoughts of self-harm.
Postpartum anxiety is less well-known but equally common. It involves excessive worry, racing thoughts, difficulty relaxing, and sometimes physical symptoms like a racing heart or nausea.
Postpartum psychosis is rare (affecting roughly 1 in 1,000 mothers) but is a psychiatric emergency. Symptoms include hallucinations, delusions, mania, confusion, and paranoid thoughts. It requires immediate hospital treatment.
How to Support Your Mental Health
- Talk openly with your partner, family, or friends about how you are feeling.
- Prioritise sleep wherever possible — sleep deprivation significantly impacts mental health.
- Get outside daily, even for a short walk. Exposure to natural light helps regulate your circadian rhythm.
- If you are struggling, contact your GP, health visitor, or a helpline such as the Postpartum Support International helpline (1-800-944-4773) or the PANDAS Foundation in the UK (0808 196 1776).
- Remember: seeking help is a sign of strength, not weakness. Treatment works, and you deserve to feel well.
Postpartum Recovery Essentials
Having the right items on hand can make a meaningful difference to your comfort during recovery. Here are some essentials that many new mums find helpful:
- Maternity pads: Heavy-duty pads for the first few weeks of lochia.
- Peri bottle: A squeeze bottle to rinse the perineal area with warm water after using the toilet.
- Comfortable, supportive underwear: High-waisted styles that sit above a caesarean scar are ideal.
- Belly wrap or support band: Provides gentle compression and support for your abdomen. See our review of the best postpartum belly wrap to find the right option.
- Nursing pillow and breast pads: Essential if breastfeeding.
- Stool softener: Speak to your pharmacist about options to prevent constipation.
- Ice packs or cooling pads: For perineal swelling and discomfort.
- A good water bottle: Staying hydrated is critical, especially if breastfeeding.
Shop Postpartum Recovery Essentials on Amazon
FAQ: Postpartum Recovery
How long does postpartum recovery take?
Most women need at least 6–12 weeks for initial physical recovery, though full healing — including core and pelvic floor rehabilitation, hormonal regulation, and emotional adjustment — can take 6–12 months or longer. Caesarean recovery generally takes longer than vaginal birth recovery. Every woman's timeline is different, and there is no single "normal."
When can I start exercising after giving birth?
Gentle pelvic floor exercises and short walks can usually begin within the first week. Most GPs will assess you at your six-week postnatal check-up before advising on further exercise. High-impact activities like running should be delayed until at least 12 weeks postpartum, ideally after a pelvic floor assessment.
Is it normal to still look pregnant weeks after giving birth?
Absolutely. Your uterus takes approximately six weeks to return to its pre-pregnancy size, and it can take much longer for abdominal muscles and skin to recover. Diastasis recti (abdominal separation) is very common and contributes to the postpartum belly appearance. Be patient and focus on recovery rather than aesthetics.
How do I know if I have postnatal depression?
Key signs include persistent low mood lasting more than two weeks, loss of interest in activities you usually enjoy, difficulty bonding with your baby, changes in sleep or appetite beyond what the baby causes, feelings of guilt or worthlessness, and withdrawing from others. If you recognise these signs in yourself, please reach out to your GP or midwife. Postnatal depression is treatable and recovery is very possible.
When is it safe to have sex after giving birth?
There is no fixed rule, but most healthcare providers suggest waiting until after your six-week postnatal check-up and until you feel physically and emotionally ready. If you had stitches, wait until they have fully healed. Use lubrication, as postnatal hormonal changes (especially with breastfeeding) can cause vaginal dryness. If sex is painful, speak to your GP — this is a common and solvable issue, often linked to pelvic floor tension.
What should I eat during postpartum recovery?
Focus on nutrient-dense foods that support healing: lean protein (eggs, chicken, fish, legumes), iron-rich foods (red meat, spinach, lentils), calcium (dairy, fortified plant milks), fibre (wholegrains, fruits, vegetables), and healthy fats (avocado, nuts, olive oil). If breastfeeding, you need approximately 500 extra calories per day. Stay well-hydrated — water, herbal teas, and broths all count.
Sources
-
American College of Obstetricians and Gynecologists (ACOG). "Optimizing Postpartum Care." ACOG Committee Opinion No. 736, May 2018. https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2018/05/optimizing-postpartum-care
-
National Institute for Health and Care Excellence (NICE). "Postnatal Care." NICE Guideline NG194, April 2021. https://www.nice.org.uk/guidance/ng194
-
Sperstad, J.B., Tennfjord, M.K., Hilde, G., Ellström-Engh, M., & Bø, K. "Diastasis recti abdominis during pregnancy and 12 months after childbirth: prevalence, risk factors and report of lumbopelvic pain." British Journal of Sports Medicine, 50(17), 1092–1096, 2016.
-
Woodley, S.J., Lawrenson, P., Boyle, R., et al. "Pelvic floor muscle training for preventing and treating urinary and faecal incontinence in antenatal and postnatal women." Cochrane Database of Systematic Reviews, 2020.
-
Donnelly, G.M., & Goom, T. "Returning to Running Postnatal — Guidelines for Medical, Health and Fitness Professionals Managing this Population." 2019. https://www.running-physio.com/postnatal-guide/
-
Gavin, N.I., Gaynes, B.N., Lohr, K.N., et al. "Perinatal Depression: A Systematic Review of Prevalence and Incidence." Obstetrics & Gynecology, 106(5), 1071–1083, 2005.
-
Richter, D., Krämer, M.D., Tang, N.K.Y., Montgomery-Downs, H.E., & Lemola, S. "Long-term effects of pregnancy and childbirth on sleep satisfaction and duration of first-time and experienced mothers and fathers." Sleep, 42(4), 2019.
-
NHS. "Your Body After the Birth." National Health Service, UK. https://www.nhs.uk/conditions/baby/support-and-services/your-body-after-the-birth/
-
Centers for Disease Control and Prevention (CDC). "Depression Among Women." https://www.cdc.gov/reproductivehealth/depression/
This article is for informational purposes only and does not replace professional medical advice. Always consult your GP, midwife, or healthcare provider with concerns about your postpartum recovery.
Visual Guide Gallery
Walking Pad vs Treadmill
30-second comparison